As high deductibles continue to increase in 2021, revenue cycle management companies (RCM) face the time-consuming and costly process of having to directly collect payments from patients, arguably the most difficult aspect of the revenue cycle. Our analysis of medical practices’ cash flow shows that high deductibles in the first six months of the year can affect an entire year’s financial health and performance due to its dependence on patient payments, creating hours of effort for revenue cycle management companies (RCM).
Time-consuming and ineffective patient financial engagement methods, such as sending paper bills and making collection calls, have long failed both patient and provider. Patient collection rates are often below 50%. Furthermore, 75% of patients stated they would leave a provider for a better payment experience*. Innovative revenue cycle management companies (RCM) must embrace new digital strategies that deliver high payment rates and a positive patient experience. Below are three proven strategies to lessen the burden and ease the cost of collecting patient payments and freeing your team to focus on more complex issues.
Offer a Modern Payment Experience
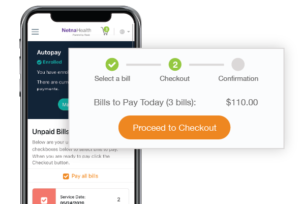 The consumerization of healthcare is here. From telehealth to virtual intake, new digital technologies are creating efficiencies and competitive advantages for early adopters. Patient billing and payment processes are a segment of the patient journey where modernization directly impacts practice cash flow. Innovative revenue cycle management companies (RCM) that enhance their customers’ patient payment experience with comprehensive digital bills and a broad range of payment options can increase payment collection rates to over 90% while maintaining customer satisfaction scores that consistently reach 100%.
The consumerization of healthcare is here. From telehealth to virtual intake, new digital technologies are creating efficiencies and competitive advantages for early adopters. Patient billing and payment processes are a segment of the patient journey where modernization directly impacts practice cash flow. Innovative revenue cycle management companies (RCM) that enhance their customers’ patient payment experience with comprehensive digital bills and a broad range of payment options can increase payment collection rates to over 90% while maintaining customer satisfaction scores that consistently reach 100%.
Payment Automation
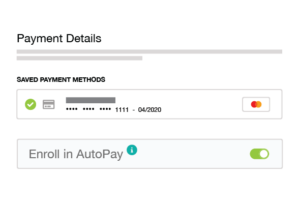 Payment automation may sound complex — driven by AI or highly customized software — but it’s really not. AI and automation can be deployed quickly and is highly stable to meet the needs of any practice, hospital, or health system. Automation solves many issues associated with the patient collection, by understanding how best to communicate with patients at a personal level. Successfully implementing payment automation while can improve patient relations while increasing cash flow, decreasing the cost to collect, and driving down the effort needed to manage patent interactions.
Payment automation may sound complex — driven by AI or highly customized software — but it’s really not. AI and automation can be deployed quickly and is highly stable to meet the needs of any practice, hospital, or health system. Automation solves many issues associated with the patient collection, by understanding how best to communicate with patients at a personal level. Successfully implementing payment automation while can improve patient relations while increasing cash flow, decreasing the cost to collect, and driving down the effort needed to manage patent interactions.
Digital Patient Outreach
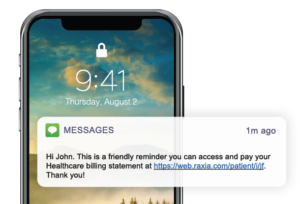 The most time-consuming effort in the traditional patient collection process is outreach. Making calls and sending paper statements have long proven ineffective. Instead, sending digital notifications using a patient’s preferred communications method — be it email, text message, voice, or chat — increases the likelihood of a successful payment. Not only will this increase the patient collection rate, it will also reduce the average number of days patient bills remain in accounts receivable and dramatically lower the cost to collect patient payments.
The most time-consuming effort in the traditional patient collection process is outreach. Making calls and sending paper statements have long proven ineffective. Instead, sending digital notifications using a patient’s preferred communications method — be it email, text message, voice, or chat — increases the likelihood of a successful payment. Not only will this increase the patient collection rate, it will also reduce the average number of days patient bills remain in accounts receivable and dramatically lower the cost to collect patient payments.
*Meddata 2020 Medical Billing Statistics