At some point, every RCM leader faces the same question: when patient call volume becomes a problem, do you hire more staff, outsource the function, or invest in AI?
For years, outsourcing was the default answer. Hand the problem to a third-party call center, pay per agent or per hour, and get it off your plate. But the math and the patient experience rarely worked out as well as expected.
Now AI has entered the conversation, and the decision has gotten more nuanced. This framework breaks down both options so you can make a confident, informed decision for your organization.
The Core Problem Both Options Are Trying to Solve
Patient billing support is expensive, repetitive, and hard to scale. The average RCM team fields a constant stream of calls and messages from patients asking the same types of questions: What’s this bill for? Was my insurance applied? Can I set up a payment plan? Why is the amount different than what I expected?
These questions are predictable. They’re also time-consuming. When your staff spends 70% of their day answering routine billing inquiries, they’re not doing the higher-value work that grows your business.
Both outsourcing and AI try to solve this. But they do it in fundamentally different ways, with very different outcomes.
The Case for Outsourcing (And Why It Falls Short)
Outsourcing to a third-party patient support center has real appeal on paper. You offload the staffing problem, get 24/7 coverage, and convert a fixed cost into a variable one.
But here’s what RCM leaders consistently report once they’re in it:
The cost is higher than expected. US-based patient support agents typically run $6 to $9 per call. That sounds manageable until you multiply it by thousands of calls per month across dozens of provider clients. It adds up fast—and it scales linearly with volume, meaning growth increases your cost burden proportionally.
Quality is inconsistent. Third-party agents are not your staff. They don’t know your clients’ specialties, their billing nuances, or the context a patient needs to understand an anesthesiology bill versus a lab bill. Inconsistent answers lead to repeat calls, escalations, and frustrated patients.
You lose visibility. When a third party handles patient interactions, you often lose insight into what patients are asking, what’s causing confusion, and where billing workflows are breaking down. That’s data you need.
It doesn’t actually fix the problem. Outsourcing is a staffing solution, not a workflow solution. The root causes, paper-heavy processes, reactive communication, and patient confusion about medical bills, remain unresolved.
The Case for AI (And What It Actually Delivers)
AI-powered patient support, done well, addresses the problem differently. Instead of adding more people to answer the same questions, it removes the need for most of those interactions to reach a person in the first place.
Raxia’s Rae AI handles patient inquiries by voice or chat, connecting directly to your health IT systems to deliver accurate, personalized, and empathetic responses. No hold times. No inconsistent messaging. Available 24/7.
Here’s what that looks like in practice:
Containment rates of 70–85%. That means 7 to 8.5 out of every 10 patient inquiries are fully resolved by AI—without ever reaching a human agent. Patients get their question answered, their payment processed, or their payment plan set up, all in a single interaction.
Cost per interaction around $0.85. Compared to $6–$9 for a US-based agent, that’s an 85–90% reduction in per-call cost. For a mid-size RCM company handling 5,000 patient calls per month, that’s the difference between $35,000–$45,000/month and roughly $4,250/month for the AI-contained interactions.
Consistency at scale. Every patient gets the same accurate information, the same tone, the same explanation—regardless of time of day or call volume. No training drift, no bad days, no turnover gaps.
Specialty-aware responses. Unlike a generalist call center agent, AI can be configured to understand the specific context of anesthesiology billing, radiology, hospital-based care, and other specialties where patients routinely don’t recognize the provider or understand the charge.
Real-time visibility. Every interaction generates data. You can see exactly what patients are asking, what’s driving confusion, and where your billing communication needs refinement. That intelligence makes your entire operation smarter over time.
The Right Model: AI on the Front Line, Humans Where It Matters
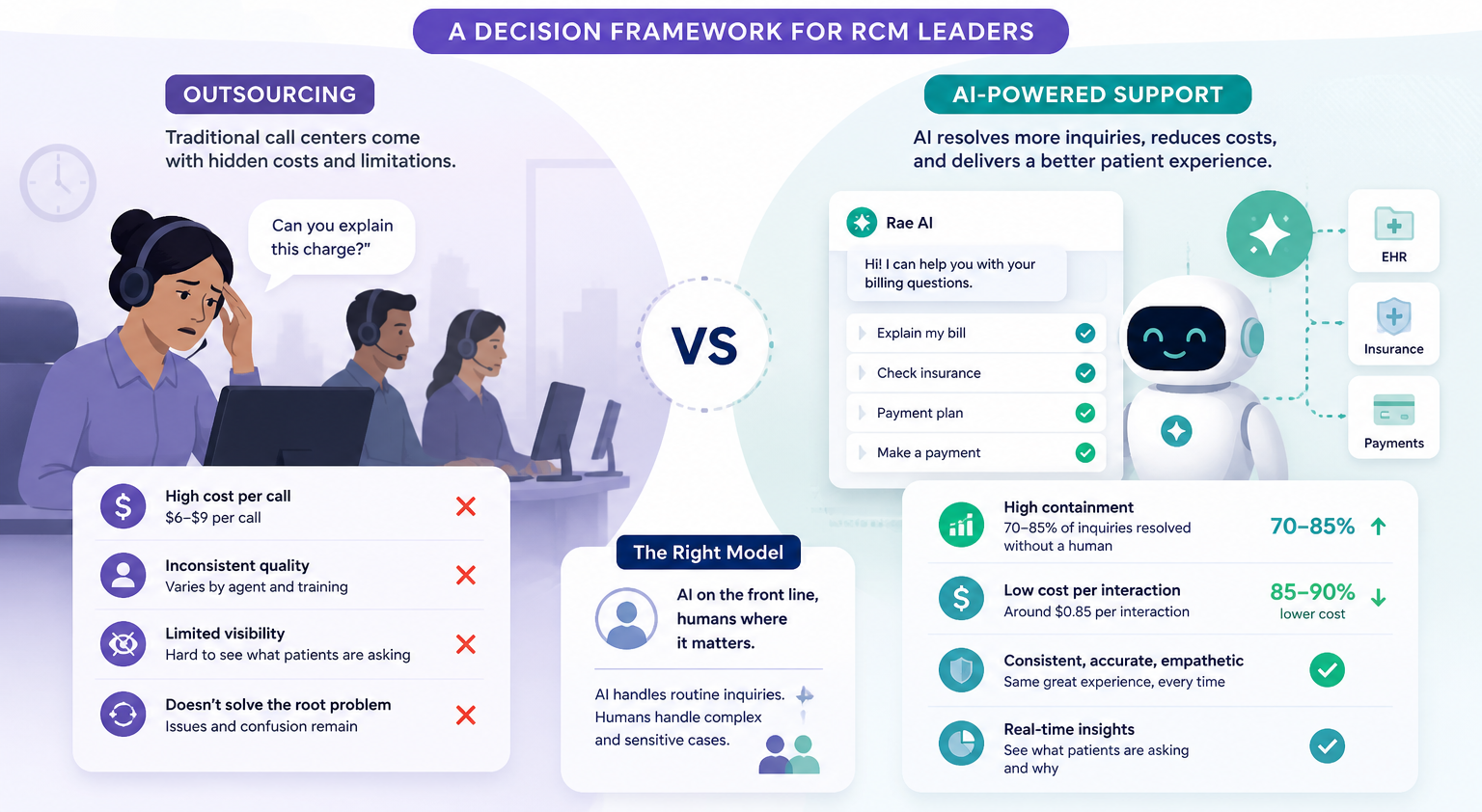
The best RCM organizations aren’t choosing between AI and people. They’re using AI to triage and resolve routine inquiries, and routing complex or sensitive cases to trained staff.
This hybrid approach means:
- AI handles balance inquiries, charge explanations, payment plan setup, insurance verification questions, and payment processing
- Humans handle disputes, hardship cases, multi-issue accounts, and situations that require judgment and empathy beyond a defined workflow
The result is a smaller, more focused patient support team doing higher-value work—while patients get faster, more consistent service around the clock.
Questions RCM Leaders Should Be Asking
Before deciding which path to take, consider:
- What is your current cost per patient interaction? If you don’t know this number, it’s worth calculating before your next contract renewal.
- What percentage of patient calls are routine vs. complex? In most RCM environments, 70–80% of inbound inquiries are repetitive and predictable—exactly the type AI handles best.
- How much visibility do you have into what patients are asking? If your outsourced team is handling calls without feeding you data, you’re flying blind.
- What happens to your unit economics as you grow? Outsourcing costs scale with volume. AI costs don’t.
- What is patient satisfaction scoring for your current support model? If CSAT is low, it’s usually a consistency and context problem—one AI solves structurally.
Final Thought
Outsourcing patient support made sense when AI wasn’t capable of delivering reliable, context-aware, HIPAA-compliant patient interactions. That time has passed.
The RCM companies seeing the biggest gains right now aren’t spending more on agents, they’re deploying AI that contains the majority of patient inquiries at a fraction of the cost, and freeing their teams to focus on the work that actually requires human judgment.
The question for RCM leaders today isn’t whether AI can handle patient support. It’s whether you can afford to wait any longer to find out.